About
The Every Breath Counts Coalition is the world’s first public-private partnership with an ambitious goal: to dramatically reduce the number of children and adults dying from pneumonia by 2030 by closing critical gaps in pneumonia prevention, diagnosis, and treatment.
Our network of UN agencies, non-government organizations, government and foundation donors, companies, and academic institutions are supporting governments in countries with some of the highest burdens of pneumonia, and are dedicated to preventing hundreds of thousands of pneumonia deaths each year.
Identifying the most vulnerable adults and children and ensuring that they receive proven, high-impact interventions at every level of the health system is the most effective strategy to close the critical gaps in pneumonia prevention, diagnosis, and treatment and save lives.
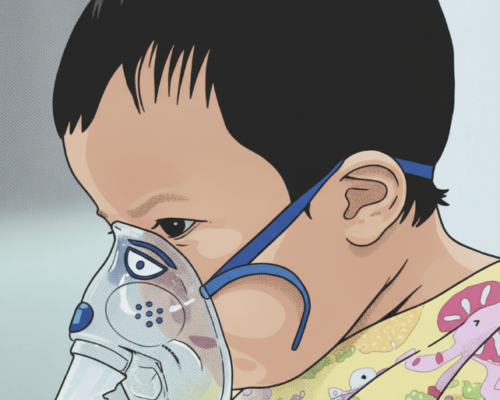
In most countries expanding coverage of the pneumonia-fighting vaccines (DTP, Hib, PCV, measles, flu, and COVID-19) will be a top priority as coverage rates are often very low. In other countries improving access to proper diagnosis and treatment with better tools like pulse oximetry and increased access to child-friendly antibiotics, oxygen, and therapeutic foods will be crucial.
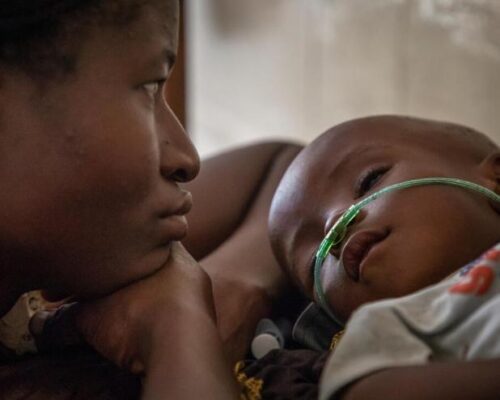
Working directly with mothers and families to improve child nutrition, household air quality, and hand washing with soap will strengthen prevention. Increasing the education, incomes, and agency of mothers with small children will advance child health and boost development everywhere.
Although pneumonia deaths are concentrated in 20 countries representing all regions and income levels, Every Breath Counts focuses on the specific challenges of reducing pneumonia deaths among the most vulnerable populations of children and adults in low- and middle-income countries where health systems are weaker. There is a particularly large and vulnerable group of children living in Nigeria, Chad, the Democratic Republic of Congo, South Sudan, Ethiopia, Somalia and Kenya who are at greatest risk of death from pneumonia.
In these countries, closing the critical gaps in pneumonia prevention, diagnosis, and treatment can save the greatest number of lives and accelerate achievement of the Sustainable Development Goals for health by 2030. Find out more about the 20 countries where pneumonia deaths are concentrated and the seven countries across Africa that are a hotspot for child pneumonia deaths.
Find out more about our members and our initiatives and email Leith Greenslade, Coordinator, Every Breath Counts Coalition, if you would like to join – leith@justactions.org.
Specific Every Breath Counts activities include:
-
-
- Ensuring countries have national strategies to control pneumonia based on local cause-of-death and risk data, to save lives now and prepare for the next respiratory pandemic
- Increasing the domestic health resources and international development assistance allocated to pneumonia-related interventions (e.g., vaccination, nutrition, clean air, diagnosis with pulse oximetry and new diagnostic tools, and access to recommended antibiotics and oxygen treatments)
- Supporting country efforts to prioritize pneumonia in applications for funding from international health and development agencies (e.g., Gavi, the Global Fund, and the Global Financing Facility for Women, Children and Adolescents)
- Accelerating introduction of the PCV vaccine in countries with no coverage and increasing efforts to lift coverage to above 90% in low-coverage countries
- Advancing Universal Health Coverage (UHC) schemes that fully cover the costs of pneumonia vaccines, diagnostic and treatment services, including improved diagnostic tools, pulse oximetry, recommended antibiotics, and oxygen therapies
- Including pneumonia diagnostic and treatment tools and therapies on World Health Organization (WHO) guidance to national governments, including on Essential Medicines Lists
- Increasing investments in innovations that improve the cost-effectiveness of pneumonia prevention, diagnosis, and treatment, with a special focus on supporting local entrepreneurs with sustainable business models
- Introducing advocacy campaigns to increase the investments needed to reduce pneumonia deaths by 2030, to raise awareness about pneumonia deaths among all stakeholders including the general public, and to encourage behavioral change by caregivers and healthcare workers, especially rapid care seeking for children with pneumonia symptoms
- Including a more robust set of pneumonia prevention, diagnosis, and treatment indicators in official health surveys (e.g., MICs, DHS, SPA, and SARA) and health impact tools, including the Lives Saved Tool (LiST) model
- Coordinating efforts by humanitarian agencies to reduce pneumonia mortality and testing new approaches to pneumonia prevention, diagnosis, and treatment in fragile settings
- Increasing research to better identify the predictors of severe pneumonia and the children and adults who are at greatest risk of death without urgent action
-
Financing Maternal RSV Immunization Through Reduced-Dose PCV Schedules
Pneumonia remains the leading infectious cause of death among children under five, accounting for more than 600,000 deaths annually worldwide. Despite gains in vaccine coverage, progress reducing pneumonia deaths has slowed, and many countries face increasingly constrained health budgets. At the same time, new tools...
05 June, 2026The power of civil society to support new vaccine introductions
Something extraordinary has been happening for the children of Chad, Somalia, and South Sudan. An unprecedented period of child health progress with the introduction of new vaccines against pneumonia, diarrhea, and malaria. Together, these three infections caused 86,000 deaths in 2021 – 45% of all...
22 June, 2025Best Practices for Pulse Oximeter Use!
“Functional, good-quality pulse oximeters should be available in every area where patients are clinically assessed or admitted in sufficient quantities to meet all needs,” The Lancet Global Health Commission on Medical Oxygen Security Do you want to improve the use of pulse oximetry among children...
06 June, 2025Climate change and respiratory health
Climate Change and Respiratory Health, brought together four leading experts – Heather Adair-Rohani from the World Health Organization (WHO), Rebecca Nantanda from Makerere University Lung Institute, Laura-Jane Smith from the British Thoracic Society, and John Sampson from Johns Hopkins University to explore different facets of...
11 December, 2024Open Letter to The Global Fund Board: Access to medical oxygen
Dear Global Fund Board, The Global Fund must continue its vital work helping eligible countries close the massive gaps in access to medical oxygen that are stymying efforts to achieve the Sustainable Development Goals (SDGs) and prepare for the next pandemic. Oxygen is an essential...
19 November, 2024Medical oxygen and the SDGs
“Apart from oxygen, name one other essential medicine that is a topline treatment for all but one of the conditions targeted by the health SDGs?” This was the focus of the second of three High Stakes Conversations on the role of medical oxygen and global...
09 July, 2024